Early Signs of Mycosis Fungoides: What You Need to Know
Mycosis fungoides is a rare form of skin cancer often mistaken for common skin conditions like eczema. Recognizing its early signs can lead to earlier intervention and better outcomes. This guide highlights the key symptoms, risk factors, and steps to take if you notice persistent skin changes.
What Is Mycosis Fungoides?
Mycosis fungoides is a rare type of cutaneous T-cell lymphoma, a cancer that begins in the white blood cells and affects the skin. The disease typically progresses slowly, often starting with symptoms that mimic benign skin conditions, such as eczema or psoriasis. This resemblance leads to frequent misdiagnosis in its early stages. Recognizing mycosis fungoides as a form of lymphoma is crucial for appropriate management and care, distinguishing it from more common dermatological issues.
Early Signs and Symptoms
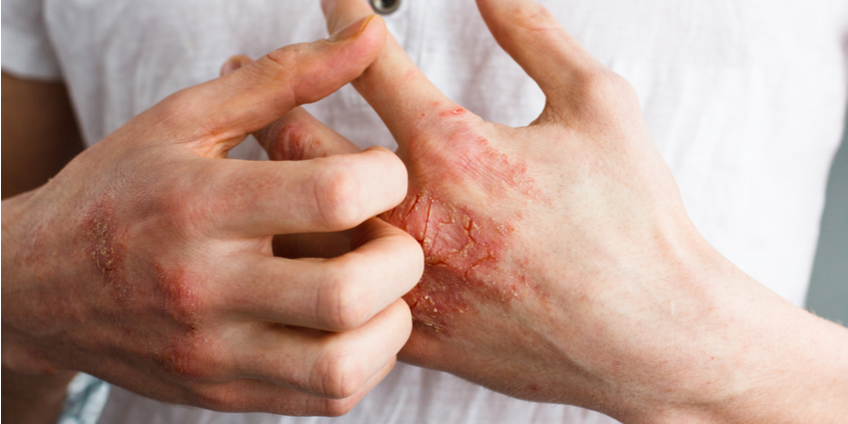
The early symptoms of mycosis fungoides often include persistent patches or plaques on the skin. These may appear as flat, scaly areas that are slightly raised and can be itchy. Color changes in the affected skin are also common, with patches appearing redder or more discolored than the surrounding skin. Because these signs can easily be mistaken for eczema, psoriasis, or other common skin conditions, they often go unnoticed or are misdiagnosed. Visual signs that deserve attention include patches that persist despite treatment with typical eczema or psoriasis medications, or patches that gradually change in size, shape, or color over time.
Who Is at Risk?
While mycosis fungoides can affect anyone, certain factors may increase the risk of developing this condition. These include age, with older adults being more frequently diagnosed, and genetics, as a family history of lymphoma or related conditions might elevate risk. Environmental exposures, such as to certain chemicals or pollutants, have also been suggested as potential risk factors, although more research is needed in this area. It is important to remember that having these risk factors does not guarantee the development of mycosis fungoides, but awareness can aid in earlier detection and management.
Mycosis Fungoides vs. Common Skin Conditions
Mycosis fungoides is often confused with common skin conditions like eczema and psoriasis due to similar symptoms such as redness, itching, and scaly patches. However, there are key differences. Eczema typically appears in skin folds and is often linked to allergies or irritants, while psoriasis usually presents as thicker, raised plaques with silvery scales, commonly on the elbows, knees, and scalp. Mycosis fungoides, in contrast, may not respond to typical treatments for these conditions and can persist or worsen over time. The persistence and unique distribution of symptoms, along with a lack of response to standard treatments, should raise suspicion for mycosis fungoides.
What to Do If You Notice Symptoms
If you notice unexplained skin changes, such as persistent patches, color variations, or unusual itching, it is important to take prompt action. The first step is to consult a dermatologist, a doctor specializing in skin conditions. Before your appointment, document your symptoms by taking photos and noting when they started and how they have changed. A dermatologist may perform a biopsy, which involves taking a small sample of the affected skin for laboratory analysis. This is the most definitive way to diagnose mycosis fungoides and rule out other conditions. Early diagnosis is crucial for effective management.
Treatment and Prognosis
Treatment options for mycosis fungoides vary depending on the stage and severity of the disease. Topical therapies, such as corticosteroids and phototherapy, are often used in early stages to manage skin symptoms. Advanced interventions, including systemic medications, radiation therapy, and stem cell transplantation, may be considered for more advanced cases. Early detection plays a significant role in improving outcomes, as it allows for timely intervention and management of symptoms. While mycosis fungoides is a chronic condition, many patients can lead fulfilling lives with appropriate treatment and regular monitoring by a healthcare team.